Diaper Rash vs. Fungal Infection: Identification & Safe Treatment Guide
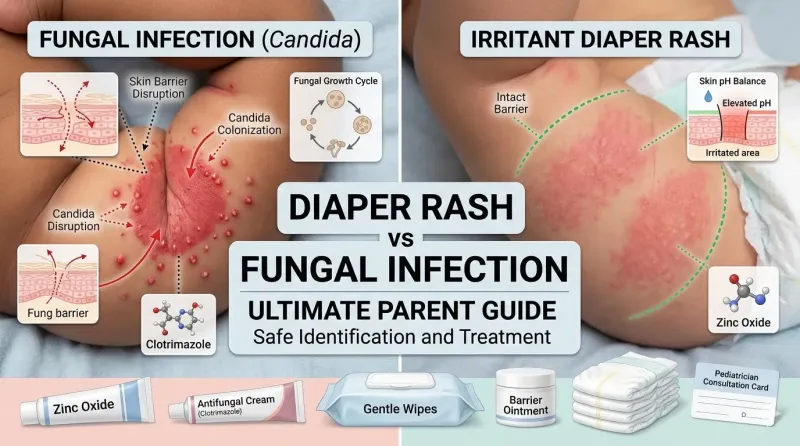
Every parent has faced it: the heart-wrenching sight of their baby's uncomfortable, red, irritated bottom. Diaper rash is one of the most common concerns in infant care, affecting up to 50% of babies at some point during their diaper-wearing years. But what many parents don't realize is that not all diaper rashes are created equal—and treating a fungal infection with regular diaper rash cream (or vice versa) can actually make the problem worse.
Understanding the critical differences between common diaper rash (irritant contact dermatitis) and fungal infections (candidal diaper dermatitis) is essential for providing your baby with the right treatment and relief. While both conditions cause discomfort and redness in the diaper area, they have distinct causes, appearances, and treatment requirements that parents must recognize to ensure proper care.
This comprehensive guide will walk you through everything you need to know about identifying, treating, and preventing both conditions. You'll learn the telltale signs that distinguish a simple irritant rash from a yeast infection, discover evidence-based treatment options that are safe for your baby's delicate skin, and understand exactly when it's time to call your pediatrician. Whether you're a first-time parent navigating diaper rash for the first time or an experienced caregiver dealing with a persistent rash that won't clear up, this guide will empower you with the knowledge to make informed decisions about your baby's care.
Understanding the Basics: What Causes Each Condition
Before diving into identification and treatment, it's crucial to understand what causes each type of rash. This foundational knowledge will help you recognize why they require different approaches.
Common Diaper Rash (Irritant Contact Dermatitis)
What It Is:
Common diaper rash, medically known as irritant contact dermatitis, is an inflammatory skin reaction caused by prolonged exposure to moisture, friction, and irritants in the diaper area.
Primary Causes:
- Prolonged moisture: Urine and stool break down the skin's protective barrier
- Friction: Rubbing from diapers against sensitive skin
- Chemical irritants: Enzymes in stool, ammonia from urine breakdown
- Infrequent diaper changes: Extended contact with wet or soiled diapers
- Introduction of new foods: Changes in stool composition and frequency
- Antibiotic use: Can disrupt normal bacterial balance
- Sensitive skin: Some babies have more reactive skin than others
How It Develops:
The skin in the diaper area is naturally more delicate than other areas of the body. When exposed to moisture for extended periods, the skin's protective outer layer (stratum corneum) breaks down. This makes it more susceptible to friction damage and penetration by irritants, leading to inflammation, redness, and discomfort.
Fungal Infection (Candidal Diaper Dermatitis)
What It Is:
Fungal diaper rash, also called candidal diaper dermatitis or yeast infection, is caused by an overgrowth of Candida albicans, a type of yeast that naturally lives on the skin and in the digestive tract.
Primary Causes:
- Candida overgrowth: The yeast multiplies excessively in warm, moist environments
- Antibiotic use: Kills beneficial bacteria that normally keep yeast in check
- Weakened immune system: Makes babies more susceptible to fungal overgrowth
- Prolonged moisture: Creates ideal environment for yeast growth
- Warm temperatures: Yeast thrives in warm, humid conditions
- Recent illness: Can disrupt normal skin flora
- Maternal yeast infection: Can be transmitted during birth
How It Develops:
Candida albicans is normally present in small amounts on the skin and in the gastrointestinal tract. However, when conditions are favorable—warmth, moisture, and disruption of normal bacterial balance—the yeast can multiply rapidly and invade the skin, causing infection. The warm, moist environment of the diaper area provides the perfect breeding ground for this overgrowth.
Key Differences in Development
| Factor | Common Diaper Rash | Fungal Infection |
|---|---|---|
| Primary Cause | Irritation from moisture/friction | Yeast overgrowth |
| Onset | Gradual, after prolonged exposure | Can develop quickly, often after antibiotics |
| Environment | Wet/dirty diapers | Warm, moist conditions |
| Risk Factors | Infrequent changes, sensitive skin | Antibiotics, weakened immunity |
Visual Identification: Spotting the Differences
Accurate identification is the first step toward effective treatment. Here's how to distinguish between common diaper rash and fungal infection by examining the rash's appearance, location, and characteristics.
Common Diaper Rash: Visual Characteristics
Appearance:
- Color: Pink to bright red patches
- Texture: Skin may appear shiny, slightly swollen, or have a "raw" appearance
- Severity: Mild cases show slight redness; severe cases may have raised bumps or small blisters
- Borders: Generally diffuse, blending into surrounding skin
Location Pattern:
- Convex surfaces: Primarily affects areas that touch the diaper most directly
- Common areas: Buttocks, thighs, genital area
- Skin folds: Typically SPARES the creases and folds (this is a KEY distinguishing feature)
- Distribution: Symmetrical, affecting both sides equally
Progression:
- Develops gradually over 1-3 days
- Worsens with continued exposure to moisture
- Improves within 2-3 days of proper treatment
Fungal Infection (Yeast): Visual Characteristics
Appearance:
- Color: Bright red, often described as "beefy red" or "angry-looking"
- Texture: Raised, may have a slightly shiny or glazed appearance
- Satellite lesions: Small red spots or pustules surrounding the main rash (THIS IS A HALLMARK SIGN)
- Borders: Well-defined, raised borders that are clearly demarcated from normal skin
- Scaling: May have slight scaling or peeling at the edges
Location Pattern:
- Skin folds: DEEPLY involves creases and folds (KEY distinguishing feature)
- Common areas: Deep creases of thighs, genital folds, between buttocks
- Can spread: May extend beyond diaper area to abdomen or thighs
- Asymmetrical: May affect one side more than the other
Progression:
- Can develop rapidly, sometimes overnight
- Often appears after antibiotic use
- Does NOT improve with regular diaper rash cream
- May worsen despite frequent diaper changes
Side-by-Side Comparison Chart
| Feature | Common Diaper Rash | Fungal Infection |
|---|---|---|
| Color | Pink to red | Bright, beefy red |
| Skin Folds | Usually spared | Deeply involved |
| Borders | Diffuse, blended | Sharp, well-defined |
| Satellite Lesions | Absent | Present (key sign) |
| Texture | Smooth, shiny | Raised, may scale |
| Response to Regular Cream | Improves in 2-3 days | No improvement or worsens |
| Onset | Gradual (1-3 days) | Rapid (can be overnight) |
Visual Red Flags: When to Suspect Fungal Infection
Seek medical evaluation if you notice:
- ✓ Rash in skin folds/creases
- ✓ Bright red, "angry" appearance
- ✓ Small red spots around the main rash (satellite lesions)
- ✓ No improvement after 3 days of regular diaper rash treatment
- ✓ Rash appeared after antibiotic use
- ✓ Rash is spreading or worsening
Symptom Comparison: Beyond Appearance
While visual identification is crucial, symptoms and behavioral cues can also help distinguish between the two conditions.
Common Diaper Rash Symptoms
Baby's Behavior:
- Mild discomfort: Baby may be slightly fussy during diaper changes
- Crying: May cry when urine or stool contacts the rash
- Sleep: Usually sleeps normally
- Feeding: Feeding patterns typically unchanged
- Overall mood: Generally content between diaper changes
Physical Symptoms:
- Mild to moderate tenderness
- Warmth in affected area
- Skin may feel slightly rough
- No fever
- No systemic symptoms
Fungal Infection Symptoms
Baby's Behavior:
- Significant discomfort: Baby is noticeably more irritable and fussy
- Intense crying: Cries during diaper changes and when area is touched
- Sleep disruption: May have trouble sleeping due to discomfort
- Feeding changes: May feed less or be more fussy during feeding
- Overall mood: Generally more irritable throughout the day
Physical Symptoms:
- Significant tenderness and pain
- Area feels warm or hot to touch
- Skin may be raw or have open areas
- Usually no fever (unless secondary bacterial infection)
- May have oral thrush (white patches in mouth) simultaneously
Associated Conditions
Common Diaper Rash:
- Usually isolated to diaper area
- No other infections present
- May coincide with diarrhea or frequent stools
Fungal Infection:
- May have oral thrush (white patches on tongue, cheeks)
- May have yeast infection in other skin folds (neck, armpits)
- Often follows antibiotic treatment
- May coincide with recent illness
Treatment Protocols: Evidence-Based Approaches
Treating the wrong condition with the wrong medication can delay healing and potentially worsen the rash. Here's how to properly treat each condition.
Treating Common Diaper Rash
First-Line Treatment: The ABCDE Method
A - Air:
- Give baby diaper-free time (10-15 minutes, 3-4 times daily)
- Lay baby on absorbent towel or waterproof pad
- Air circulation promotes healing and keeps area dry
B - Barrier Creams:
- Zinc oxide creams: Desitin, Boudreaux's, generic brands (20-40% zinc oxide)
- Petroleum jelly: Vaseline, Aquaphor
- Lanolin-based creams: Pure lanolin or lanolin-based products
- Application: Apply thick layer (like frosting a cake) at every diaper change
C - Clean:
- Gently clean with warm water and soft cloth
- Avoid harsh soaps or alcohol-based wipes
- Pat dry gently—don't rub
- Consider using water-only cleaning for severe rashes
D - Diaper Changes:
- Change diapers frequently (every 2-3 hours)
- Change immediately after bowel movements
- Check diapers frequently during the night if rash is severe
E - Evaluate:
- Monitor for improvement within 2-3 days
- If no improvement, consider fungal infection
- Watch for signs of infection (fever, pus, worsening)
Additional Treatments:
- Hydrocortisone 0.5-1%: For severe inflammation (use sparingly, max 3-5 days, consult pediatrician)
- Antacids: Some parents use liquid antacid (like Maalox) applied to area—consult pediatrician first
- Breast milk: Some studies show breast milk application can help (apply, let air dry)
Expected Timeline:
- Mild rash: Improvement within 24-48 hours
- Moderate rash: Improvement within 2-3 days
- Severe rash: May take 4-7 days
Treating Fungal (Yeast) Infection
First-Line Treatment: Antifungal Medications
Over-the-Counter Options:
- Clotrimazole 1%: Lotrimin AF, generic brands
- Miconazole 2%: Micatin, Monistat Derm
- Nystatin: Available by prescription, very effective for Candida
Application Protocol:
- Clean and dry the area thoroughly
- Apply thin layer of antifungal cream to affected area
- Apply 2-3 times daily (or as directed)
- Continue for 7-14 days, even if rash improves sooner
- Apply barrier cream (zinc oxide) OVER antifungal after it absorbs
Important Notes:
- DO NOT use hydrocortisone with fungal infection (can worsen yeast growth)
- Complete the full course even if rash appears better
- Expect improvement within 2-3 days of starting antifungal
- If no improvement after 3-5 days, contact pediatrician
Prescription Options (if OTC fails):
- Stronger antifungals: Ketoconazole, econazole
- Combination creams: Antifungal + mild steroid (short-term use only)
- Oral antifungals: For severe or recurrent cases (fluconazole)
Treating Oral Thrush (if present):
- Nystatin oral suspension (prescription)
- Apply to inside of mouth after feeding
- Treat both diaper area and mouth simultaneously
- Sterilize pacifiers, bottle nipples daily
Supportive Care:
- Continue frequent diaper changes
- Air exposure when possible
- Keep area as dry as possible
- Avoid tight-fitting diapers or clothing
Expected Timeline:
- Initial improvement: 2-3 days
- Significant improvement: 5-7 days
- Complete resolution: 10-14 days
Combination Rashes
Sometimes babies have both irritant diaper rash AND fungal infection simultaneously. In these cases:
- Treat fungal infection first with antifungal cream
- Apply barrier cream over antifungal after it absorbs
- Continue both treatments until rash resolves
- Consult pediatrician for guidance
When to Seek Medical Attention
While most diaper rashes can be managed at home, certain situations require prompt medical evaluation.
Immediate Medical Attention (Within 24 Hours)
Contact your pediatrician immediately if:
- Fever: Temperature of 100.4°F (38°C) or higher in infants under 3 months; 102°F (38.9°C) or higher in older infants
- Signs of bacterial infection:
- Pus or yellow/green discharge
- Honey-colored crusting
- Red streaks extending from rash
- Swelling or warmth spreading beyond diaper area
- Blisters or open sores: Large blisters, open wounds, or bleeding
- Severe pain: Baby is inconsolable or in obvious severe pain
- Rapid spread: Rash spreading quickly to abdomen, back, or other areas
Schedule Appointment (Within 2-3 Days)
Make an appointment if:
- No improvement: Common diaper rash shows no improvement after 3 days of proper treatment
- Suspected fungal infection: Rash has characteristics of yeast infection
- Recurrent rashes: Baby gets frequent diaper rashes (more than 3-4 times per month)
- Uncertain diagnosis: You're unsure whether it's irritant rash or fungal infection
- Severe rash: Rash is very red, raw, or covers large area
- Oral thrush present: White patches in mouth along with diaper rash
- Recent antibiotic use: Rash appeared during or after antibiotic treatment
Emergency Room (Immediate)
Go to ER if:
- Baby appears very ill, lethargic, or unresponsive
- High fever with rash
- Signs of severe infection (rapid breathing, poor feeding, extreme fussiness)
- Rash accompanied by other concerning symptoms
Prevention Strategies: Keeping Rash at Bay
Prevention is always better than treatment. Here's how to minimize the risk of both types of diaper rash.
General Prevention for All Diaper Rashes
Diaper Change Best Practices:
- Frequency: Change diapers every 2-3 hours, even if not soiled
- Immediate changes: Change immediately after bowel movements
- Gentle cleaning: Use warm water and soft cloth or fragrance-free wipes
- Pat dry: Gently pat (don't rub) the area dry
- Air time: Give baby 10-15 minutes of diaper-free time daily
Barrier Protection:
- Apply barrier cream at every diaper change (especially at night)
- Use zinc oxide or petroleum-based products
- Apply thick enough to see a white layer
- Don't scrub off completely at each change—gently remove soiled portion and reapply
Diaper Selection:
- Choose highly absorbent diapers
- Ensure proper fit—not too tight, not too loose
- Consider fragrance-free, hypoallergenic brands if baby has sensitive skin
- Some babies do better with cloth diapers; others with disposables
Preventing Fungal Infections Specifically
During and After Antibiotics:
- Be extra vigilant with diaper changes during antibiotic treatment
- Apply barrier cream more frequently
- Consider probiotics (consult pediatrician for appropriate strain and dose)
- Watch for early signs of yeast infection
Maintain Dry Environment:
- Avoid plastic pants or waterproof covers that trap moisture
- Change wet diapers immediately
- Use super-absorbent diapers for overnight
- Allow maximum air exposure
Hygiene Practices:
- Wash hands before and after diaper changes
- Clean and sterilize pacifiers, bottle nipples daily
- Wash cloth diapers in hot water with fragrance-free detergent
- Avoid sharing towels or washcloths
Special Situations
During Diarrhea:
- Change diapers immediately after each bowel movement
- Use water instead of wipes (stool enzymes are very irritating)
- Apply thick barrier cream after every change
- Give extra air time
- Consider calling pediatrician if diarrhea persists
During Teething:
- Teething can cause looser stools, increasing rash risk
- Be extra vigilant with changes
- Increase barrier cream application
When Starting Solids:
- New foods can change stool composition and frequency
- Introduce one food at a time
- Watch for food sensitivities that cause diarrhea
- Increase diaper change frequency during transition
Natural and Home Remedies: What Works and What Doesn't
Many parents prefer natural approaches. Here's what's evidence-based and what to avoid.
Evidence-Supported Natural Remedies
Breast Milk:
- Evidence: Some studies show breast milk can be as effective as hydrocortisone for mild rashes
- How to use: Apply fresh breast milk to affected area, let air dry
- Best for: Mild irritant diaper rash
- Limitations: Not effective for fungal infections
Coconut Oil:
- Evidence: Has mild antimicrobial and moisturizing properties
- How to use: Apply thin layer as barrier
- Best for: Prevention and mild rashes
- Limitations: Not strong enough for moderate-severe rashes or fungal infections
Air Exposure:
- Evidence: Strong evidence that air exposure promotes healing
- How to use: 10-15 minutes, 3-4 times daily
- Best for: All types of diaper rash
- Limitations: Needs to be combined with other treatments
Oatmeal Baths:
- Evidence: Colloidal oatmeal has soothing, anti-inflammatory properties
- How to use: Add colloidal oatmeal to lukewarm bath water
- Best for: Soothing irritated skin
- Limitations: Supportive care only, not primary treatment
Popular but Unproven or Potentially Harmful Remedies
AVOID - Cornstarch:
- Why: Can feed yeast and worsen fungal infections
- Risk: May also be inhaled and cause respiratory issues
AVOID - Baking Soda Baths (frequent use):
- Why: Can disrupt skin's natural pH balance
- Occasional use: May be okay for soothing (1-2 tablespoons in bath), but not as primary treatment
AVOID - Essential Oils:
- Why: Can cause severe skin irritation and allergic reactions in infants
- Risk: Some essential oils are toxic to infants
- Exception: Highly diluted lavender in carrier oil may be okay for older babies, but consult pediatrician first
AVOID - Vinegar:
- Why: Too acidic for baby's delicate skin
- Risk: Can cause chemical burns and worsen irritation
CAUTION - Herbal Creams:
- Why: Not regulated, may contain allergens or irritants
- Recommendation: Consult pediatrician before using any herbal product
Special Considerations
Cloth Diapers vs. Disposables
Cloth Diapers:
- Pros: More breathable, less chemical exposure, cost-effective
- Cons: Require more frequent changes, proper washing essential
- Best practices:
- Change every 1-2 hours
- Wash in hot water with fragrance-free detergent
- Rinse thoroughly to remove all detergent residue
- Avoid fabric softeners (can reduce absorbency and irritate skin)
- Sun-dry when possible (UV light has natural disinfecting properties)
Disposable Diapers:
- Pros: More absorbent, convenient, may reduce rash frequency
- Cons: More expensive, environmental concerns, some babies sensitive to materials
- Best practices:
- Choose fragrance-free, hypoallergenic brands
- Change every 2-3 hours
- Don't overtighten
- Consider switching brands if rash persists
Recurrent or Chronic Diaper Rash
If your baby experiences frequent diaper rashes, consider:
- Underlying conditions:
- Eczema or atopic dermatitis
- Seborrheic dermatitis
- Psoriasis (rare in infants)
- Immunodeficiency
- Metabolic disorders
- Food sensitivities:
- Cow's milk protein allergy
- Other food allergies or intolerances
- Chronic diarrhea:
- May indicate underlying digestive issues
When to investigate further:
- Rash occurs more than once per month
- Rash doesn't respond to appropriate treatment
- Rash is severe or unusual in appearance
- Baby has other symptoms (poor weight gain, chronic diarrhea, frequent infections)
Frequently Asked Questions
Can I use regular diaper rash cream for a yeast infection?
No. Regular diaper rash creams (zinc oxide, petroleum jelly) create a barrier but don't kill yeast. Using only barrier cream on a fungal infection can trap moisture and actually worsen the yeast overgrowth. You need an antifungal medication (clotrimazole, miconazole, or nystatin) to treat yeast infections. Once the antifungal has absorbed, you can apply barrier cream over it.
How long should I wait before calling the doctor?
For common diaper rash: Call if no improvement after 3 days of proper home treatment.
For suspected yeast infection: Call within 1-2 days, as you'll likely need prescription or OTC antifungal medication.
Call immediately if: fever, signs of bacterial infection, blisters, severe pain, or baby appears very ill.
Can I use hydrocortisone cream for diaper rash?
For common diaper rash: Mild hydrocortisone 0.5-1% can be used sparingly for 3-5 days for severe inflammation, but consult your pediatrician first.
For fungal infection: DO NOT USE hydrocortisone alone, as it can worsen yeast growth. Only use combination products (antifungal + steroid) if specifically prescribed by your doctor, and only for short-term use.
Will my baby outgrow diaper rash?
Most babies experience diaper rash occasionally, especially during: - Teething periods - Antibiotic treatment - Introduction of solid foods - Episodes of diarrhea Frequency typically decreases as babies: - Have fewer bowel movements (after starting solids) - Spend less time in diapers (during potty training) - Develop more resilient skin Most children outgrow frequent diaper rash by 18-24 months.
Can I prevent diaper rash completely?
While you can't prevent all diaper rashes, you can significantly reduce frequency and severity by: - Changing diapers frequently - Using barrier cream preventively - Allowing air exposure - Keeping area clean and dry - Avoiding irritants (fragranced products, harsh soaps) Even with perfect care, occasional rashes may still occur due to illness, teething, or other factors beyond your control.
Is it safe to use adult antifungal cream on babies?
Some OTC adult antifungal creams (clotrimazole 1%, miconazole 2%) are safe for babies, but: - Always check with your pediatrician first - Use only as directed - Apply sparingly to affected area only - Don't use on broken skin unless directed by doctor - Never use combination antifungal/steroid creams without prescription Nystatin (prescription) is often preferred for infants as it's very gentle and specifically targets Candida.
Can diaper rash cause fever?
Simple diaper rash: No, should not cause fever.
Fungal infection: Typically does not cause fever unless there's a secondary bacterial infection.
If fever is present: This suggests: - Bacterial infection (requires immediate medical attention) - Systemic illness - Other underlying condition Contact your pediatrician immediately if diaper rash is accompanied by fever.
Conclusion: Empowered Care for Your Baby
Navigating diaper rash can be stressful for any parent, but armed with the right knowledge, you can confidently identify, treat, and prevent both common diaper rash and fungal infections. Remember these key takeaways:
Identification is Key:
- Common diaper rash: Pink/red, spares skin folds, improves with barrier cream
- Fungal infection: Bright red, involves folds, satellite lesions, needs antifungal
Treatment Must Match the Cause:
- Irritant rash: ABCDE method (Air, Barrier, Clean, Diaper changes, Evaluate)
- Yeast infection: Antifungal medication + barrier protection
- Never use steroid cream on fungal infection
Prevention is Possible:
- Frequent diaper changes are your best defense
- Barrier cream at every change prevents most rashes
- Air exposure promotes healing and prevention
- Extra vigilance during antibiotics, diarrhea, and teething
Know When to Seek Help:
- No improvement after 3 days of appropriate treatment
- Fever, pus, blisters, or severe symptoms
- Uncertain diagnosis
- Recurrent or chronic rashes
Every baby is different, and what works for one may not work for another. Trust your instincts as a parent. If something doesn't seem right, or if your baby is in significant discomfort, don't hesitate to contact your pediatrician. They're there to help you navigate these common but challenging situations.
Remember, diaper rash is temporary. With proper care, most rashes clear up within a few days to a week. Your dedication to your baby's comfort and health is making a difference, even on those challenging days and nights.
You've got this, parent. Your baby is lucky to have someone who cares enough to learn and provide the best possible care.



